Patients
Discover a better approach to pelvic pain relief

Common Symptoms Experienced by Women With
Dropped or Leaky Bladder

Lower Back Pain

Recurring UTI

Pelvic Pressure

Painful Intercourse

Vaginal Pressure

Chronic Urge to Urinate
Suffering from symptoms
Pelvic Organ Prolapse, also knows as POP, occurs when the tissues and/or muscles of a women’s pelvic floor become weak or damaged. This causes the pelvic organs (bladder, uterus, rectum and urethra) to fall downward into the vagina, similar to a hernia. Women may feel or see tissue coming out of the opening of their vagina as this progresses.
Vaginal Prolapse
Symptoms Include:
Common symptoms of POP include: Pressure and/or pain in the vagina or rectum or both, bulge(s) in the vagina or at the opening, and problems with urination or having a bowel movement .
Many factors can damage or weaken the pelvic floor. Some of the reason’s women experience prolapse are:
- Pregnancy and childbirth
- Aging and menopause
- Problems that involve repeated straining, such as chronic cough and constipation
- Obesity
- Heavy lifting
- Genetics
Pelvic Organ Prolapse, also knows as POP, occurs when the tissues and/or muscles of a women’s pelvic floor become weak or damaged. This causes the pelvic organs (bladder, uterus, rectum and urethra) to fall downward into the vagina, similar to a hernia. Women may feel or see tissue coming out of the opening of their vagina as this progresses.
Types of Pelvic Organ Prolapse
Stages of Uterine Prolapse
No prolapse
Leading edge descends
to 1 cm above hymen
Leading edge of the
prolapse remains 1 cm or
more above the hymen
Leading edge extends
over than 1 cm beyond
hymen but less than 2 cm
of total vaginal length
Complete
eversion of vaginal
Stress Urinary Incontinence Symptoms Include:
- Urine leaks out when you laugh, cough, sneeze, or exercise
- A need to urinate frequently
- Feeling an urgent need to urinate
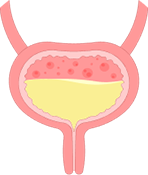
Cystitis
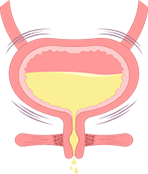
urinary incontinence
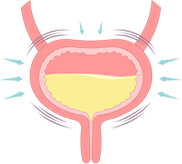
overactive bladder
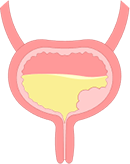
bladder cancer
bladder polyps
bladder stone


Treatment Options for Pelvic Floor Prolapse
The objectives of pelvic organ prolapse surgery are to improve a women’s quality of life while restoring normal pelvic floor function
A surgeon will repair the weakened tissue or organ as part of the surgical procedure. The surgeon may use a special non-mesh graft such as DermaPure® or VNEW® for reinforcement of the surgery.
Some types of surgery are done through an incision in the vagina. Others are done through an incision in the abdomen or with laparoscopy.
Recovery time after prolapse surgery varies depending on the type of surgery. Most patients need to take a few weeks off from work. Surgeons provide specific instructions regarding restrictions such as avoiding exercise, lifting and straining for a period of time.
Introducing VNEW Dermis and VNEW Fascia Lata, an All-Natural, Mesh-Free Solution for POP and SUI
VNEW Dermis is a next-generation biologic that uses a human tissue graft to repair weakened or damaged pelvic floor muscles. VNEW Fascia Lata supports the urethra and the bladder.
This innovative technology offers a mesh-free, all-natural solution that 9 out of 10 women prefer. VNEW is also being utilized in gender affirmation procedures and post-cancer vaginal reconstruction.




Complications with Traditional Surgery
The objectives of pelvic floor surgery include improving quality of life, restoring normal function and ensuring comfort for you, the patient. However, traditional methods can fall short:
- Synthetic mesh is a foreign material that creates substantial scarring and inflammation. It is associated with complications that can include:
- Bladder injury, mesh contraction causing vaginal tightening and pain, erosion of the mesh into the bladder or rectum, causing vaginal bleeding/discharge, pelvic or groin pain, and pain with intercourse
Native tissue repair produces scars that, while useful for supporting prolapsed tissues, can result in vaginal stenosis (narrowing of the vagina), which can cause painful sexual intercourse. Scarring can also interfere with healing.
VNEW: The better option to repair your pelvic organ prolapse, dropped bladder and leaky bladder
Rather than introducing a synthetic mesh substance that can be rejected by the body, VNEW heals by encouraging the body to incorporate the graft as part of its own tissue.
VNEW Dermis uses dCELL Technology which stimulates your own tissue to regenerate. Within a few days, VNEW begins to fuse with the body’s vasculature system, becoming a seamless part of your pelvic floor.
The result is regenerative medicine that offers lasting freedom from POP and SUI symptoms, and a return to the active life you desire.


Meet Sophie: She has Pelvic Organ Prolapse
She's waiting to see her gynecologist about something that's worrying her. Sophie's a bit embarrassed as she describes two symptoms to her doctor: 1. A sensation of pressure in her pelvic area 2. A bulge of tissue extending into her vagina.
What is dCELL® Technology?
dCELL® Technology originated in the U.K. at the University of Leeds and was first used for aortic heart valve replacement since those were prone to rejection. The process was then translated to other tissues.
DermaPure® and VNEW® tissue are created using dCELL® Technology. Unlike alternative processes, dCELL® Technology is a very gentle, process, resulting in >99% of DNA removal, without damaging the structure of the tissue.
This means that DermaPure® and VNEW® stimulate the patient’s own cells, signally the body to heal and promotes regeneration.
Why is it beneficial to remove the DNA from the tissue?
It is beneficial to the patient because it reduces the risk of a woman’s body rejecting the tissue.
Enhanced angiogenesis and integration: DermaPure® exerted a higher quantity and quality of revascularization within 3 – 4 weeks and integrates with and closely approximates the structure and function of native tissue.1,2
Reduced fibrosis: Progressive colonization of DermaPure® by native cells results in expression of key genes that are associated with reduced inflammation.²
This is important to women so they can feel confident in themselves and resume their normal lifestyle.
95% of women who had pelvic organ prolapse repair surgery with dCELL® technology would recommend it.*
*Reference: NL Guerette, Connelly JR, C Jay and JC Lukban. Safety and Anatomic E cacy of Transvaginal Prolapse Repair Augmented with a Novel Decellularized Human Dermal Allograft. AUGS, 2019.
“[Before surgery] I had increasing pain and pressure bulging into my vaginal cavity. Issues with elimination (both bowel and bladder) and consequently those issues led to insecurities with intimacy. I’m back to leading a full and active life. To the ladies out there — don’t suffer. There are solutions.”
Patty G. Patient and Registered Nurse
The Better Approach to Pelvic Floor Pain is Here
dCell® Technology has been used in thousands of pelvic floor procedures with zero complications.
- Cystocele
- Rectocele
- Enterocele
- Apical Prolapse
- Rectal Prolapse
- Synthetic Mesh Removal
- Stress Urinary Incontinence
- Fistula
- Cervical Cancer
- Complex Gender Procedures
“I wish for more women to be able to experience the amazing recovery that I’ve enjoyed and I am grateful that companies out there like ARMS offer products like DermaPure® so women like me can participate in our lives uninhibited and unencumbered by a medical condition.”
Christine V., Patient and Registered Nurse
Frequently Asked Questions
Common causes of pelvic organ prolapse include pregnancy, childbirth, hormonal changes after menopause, obesity, severe coughing, and straining on the toilet.
Pelvic organ prolapse symptoms include a feeling of pressure and/or pelvic floor pain, bulge(s) in the vagina or at the opening, painful sexual intercourse, problems with urination or having a bowel movement, and recurring urinary tract infection.
In the past, it was common to use surgical mesh in surgery. However, this method comes with considerable downsides and complications. VNEW is an all-natural mesh-free option that works for all types of pelvic floor prolapse.
The types of pelvic organ prolapse include:
- Cystocele – dropped bladder (not feeling empty after urination)
- Rectocele – bulge at the bottom of the vagina (difficulty moving bowels)
- Enterocele – herniation of the small bowel (a pulling sensation in the pelvis that eases when lying down)
- Apical Prolapse – descent of the uterus, cervix, or vaginal vault
Pelvic organ prolapse is a condition that affects the internal pelvic floor organs, causing them to shift downwards. In some cases, tissue can be seen extending from the vaginal opening.
VNEW aids in reinforcing the walls of the pelvic floor, allowing the pelvic organs to resume their correct position. Patients report less discomfort and pain after the procedure, and a return to normal activities that were not possible before surgery.
VNEW is a skin graft from donor tissue that has had more than 99% of the original DNA removed during a patented process. Studies have shown that this unique process results in less immunogenicity, a condition where foreign cells produce an unwanted immune response. This technology has been used in thousands of surgeries with no reported complications.
Urinary incontinence is when a person passes urine by accident. It is more common in older people, especially women.
There are three main types of urinary incontinence.
Stress Urinary Incontinence (SUI) is when small or moderate amounts of urine are released when pressure on your bladder increases during activities such as laughing, coughing or sneezing. SUI is a urethral problem in which VNEW Fascia Lata is a viable option.
Overactive bladder (OAB) is the beeline to the bathroom because of the sudden, uncontrollable need to pass urine. OAB is a bladder problem in which medication is prescribed to reduce the spasms.
Mixed incontinence occurs in many people who experience both SUI and OAB.
Incontinence is caused by a number of factors including:
- Pregnancy
- Childbirth
- Aging
- Prior pelvic floor surgery
- Chronic coughing
- Chronic constipation and straining
- Obesity
- Smoking
Many myths surround urinary incontinence, including that urinary incontinence is a normal part of aging, hereditary, that very limited treatment options exist, or that you can reduce your fluid intake to help manage your incontinence. The truth is that leaking urine is not an inevitable part of aging and many treatment options exist, with surgery as just one of the options. Once diagnosed, you and your doctor can decide if surgery is the right option for you.
A range of treatment options exists for urinary incontinence including:
- External pouch with catheter
- Pads or adult diapers
- Pessaries designed for SUI
- High-fiber diet
- Synthetic mesh
- Surgery with a biologic (fascia lata or dermis)
- VNEW Dermis IFU
- VNEW Fascia Lata IFU

Reclaim your freedom and boost your confidence.
Ask Your Healthcare Professional if VNEW® is Right For You
Patient Resources
- Brochure designed to help you better understand pelvic organ prolapse and treatment options.
- YouTube channel hosts a variety of patient educational videos on pelvic floor disorders.
- Fact sheets designed to help you better understand your diagnoses and treatment options.
- Educational website about pelvic floor disorders and provides an online forum for women to connect with other patients.
References
- Obstet Gynecol. 2009Dec;114(6): 1278-83. Wu JM, Hundley AF, Fulton RG, Myers ER
- NL Guerette, Connelly JR, C Jay, and JC Lukban. Safety and Anatomic Efficacy of Transvaginal Prolapse Repair Augmented With a Novel Decellularized Human Dermal Allograft. AUG 2019. dCELL® technology is a registered trademark of Tissue Regenix Limited.
- Recurrent pelvic organ prolapse: International Urogynecological Association Research by Sharif Ismail, Int Urogynecol J (2016) 27:1619-1632
